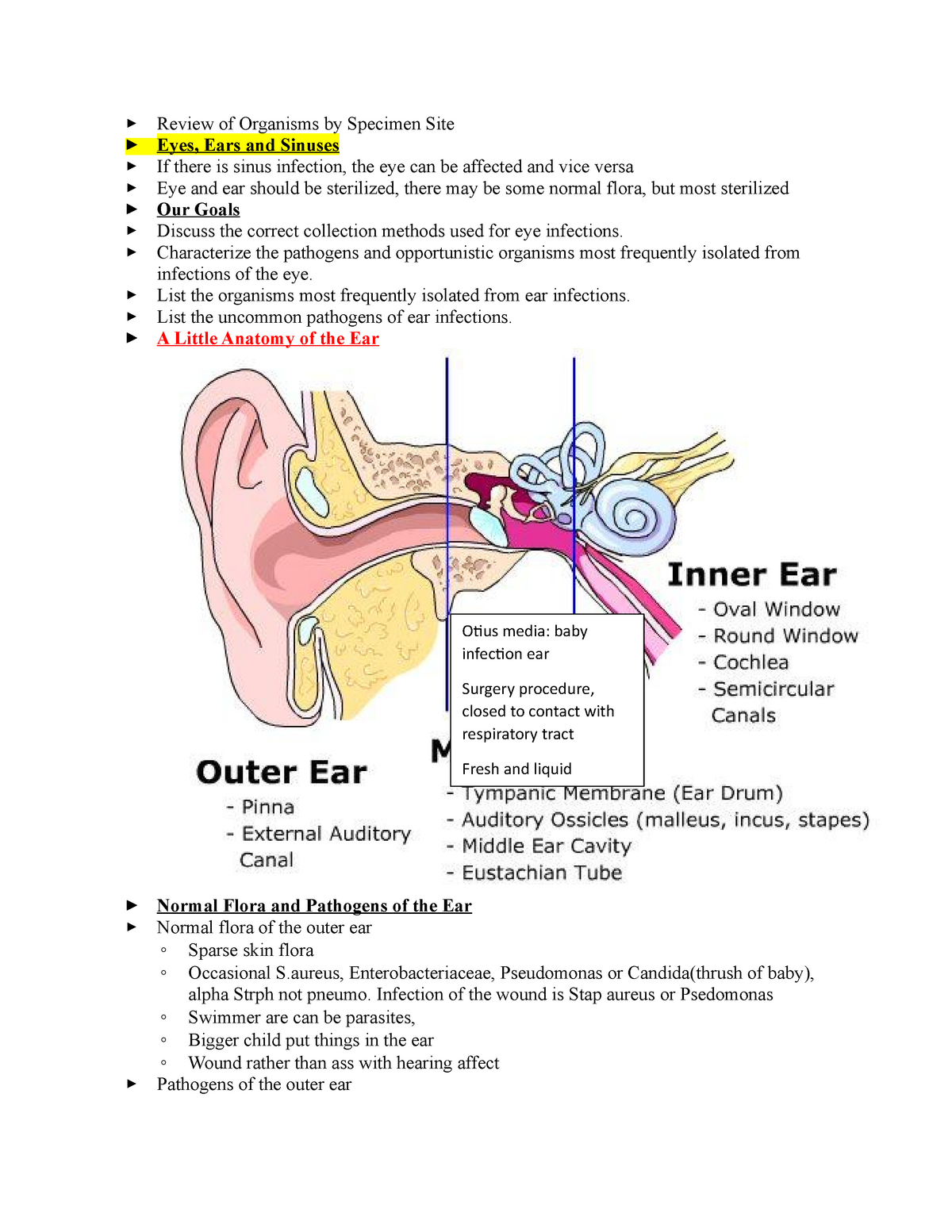
The resected portion of small bowel as well as biopsies from other GI sites showed nonnecrotizing granulomas. He was admitted at the age of 12 years to the intensive care unit with septicaemia caused by small bowel microperforations ( Figure 17) requiring small bowel resection and ileostomy. He was lost to follow-up for several years while he was treated persistently with steroids. He had a human leukocyte antigen (HLA)-matched sibling however, the family did not agree to proceed with HSCT. Prophylactic trimethoprim–sulfamethoxazole was also added. Vomiting was explained by gastric outlet obstruction, a gastrojejunal tube was inserted for feeding, and he was started on steroids for the gastrointestinal inflammation. Biopsies of the colon and rectum revealed PAS+ (Periodic acid-Shiff) staining of macrophages in the rectum that raised the possibility of CGD, a diagnosis which was later confirmed. Repeat upper- and lower-GI endoscopies no longer showed eosinophilic gastroenteritis. However, vomiting and weight loss persisted for the next 6 months. He was given the diagnosis of eosinophilic gastroenteritis and was started on omeprazole and ketotifen. Biopsies revealed a focal eosinophilic abscess in the duodenum but no granulomas. Upper gastrointestinal (GI) endoscopies revealed diffuse inflammation from the esophagus to the proximal region of the small bowel. Patient 5 presented at 3 years of age with a history of persistent nonbilious vomiting for almost 2 weeks. Engraftment and immune reconstitution are robust with complete resolution of symptoms. He underwent a matched sibling donor HSCT at 9 months of age with an uneventful course. 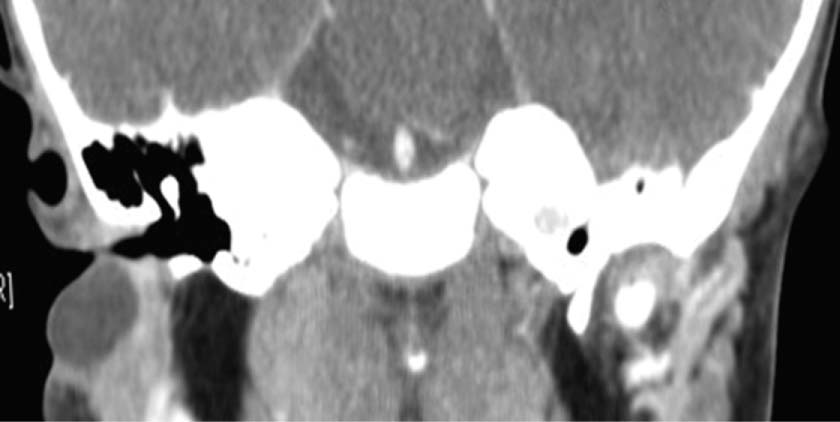
Once his lymphadenitis and fever resolved, he was discharged on trimethoprim–sulfamethoxazole and itraconazole prophylaxis, and he did well on this treatment. A CT of his chest showed multiple small pulmonary nodules ( Figure 11) and an abdominal US revealed splenomegaly with focal splenic hypoechoic lesions ( Figure 12). Given the persistence of fever, further imaging studies were performed. His infection was treated and the diagnosis of X-linked CGD was made. Cultures again grew Staphylococcus aureus and the microscopic description was again consistent with granulomatous inflammation. He was treated but presented again at 4.5 months of age with a right-sided purulent postauricular lymphadenopathy ( Figures 9 and 10) and persistent fevers. Cultures grew Staphylococcus aureus and microscopically the tissue showed granulomatous inflammation. Patient 3 presented initially at 2 months of age with left-sided cervical lymphadenopathy requiring excision and debridement. He was fully engrafted and all lesions completely resolved. He received a matched sibling donor HSCT and tolerated the procedure well. He was started on weekly interferon gamma therapy. A laparoscopic biopsy was then performed, which was negative for fungi or bacteria but showed nonnecrotizing granulomas on microscopic examination. These lesions waxed and waned over the following months. He was treated again with amphotericin and caspofungin. Six months after antifungal treatment was started, abdominal ultrasound (US, Figure 4) showed multiple splenic lesions and splenomegaly. A follow-up CT scan after 4 months of antifungal treatment showed complete resolution of the axillary lesion and a significant decrease in the number of lung lesions with stable mediastinal and hilar lymphadenopathy. He was treated with amphotericin and later with voriconazole and itraconazole. A computed tomography (CT) scan of his chest demonstrated mediastinal and hilar lymphadenopathy ( Figure 2) as well as extensive nodular lung disease ( Figure 3). This finding led to the suspicion and then confirmation of X-linked CGD. This lymph node was excised and found to grow Aspergillus in culture. He presented again at 3 years of age with an erythematous nodule with pustules on the medial aspect of his left arm with an accompanying enlarged lymph node in his left axilla ( Figure 1). Patient 1 presented with a history of cervical lymphadenitis requiring excision at 1 year of age.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
